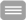EncRescue
Pathomechanisms and novel treatment strategies of sepsis-induced cognitive dysfunction
Long-term cognitive dysfunction is a common problem after surviving sepsis. Symptoms include deficits in memory and learning as well as in executive functions. These deficits may last for years or even be irreversible. Neurocognitive dysfunction after sepsis is severe and highly impairing, affecting patients but also families and caregivers. With medical progress, the number of critical ill patients and survivors of severe sepsis in intensive care units increases making long-term cognitive dysfunction to a growing public health problem. In large clinical studies up to 70% of critical ill patients have persistent neurocognitive deficits at hospital discharge and 45% continue to have neurocognitive dysfunction after one year. A recent study demonstrates that about one third of survivors at one year after discharge have persistent cognitive deficits similar to mild Alzheimer’s disease.
In contrast to the high prevalence and clinical relevance, the pathophysiology underlying cognitive deficits after severe sepsis is largely unknown. Causative therapeutic options are missing. In preliminary studies to EncRescue we established a mouse model for severe sepsis and evaluation of long-term cognitive dysfunction. We found characteristic phenotypic changes, deficits in neuronal transmission, and specific neurochemical changes in the brain of these animals. Now we aim towards development of therapeutic regimes that are target-directed and interfere with pathophysiological processes in the development and maintenance of neurocognitive dysfunction. In EncRescue we will investigate direct measures to influence pathogenic gene regulation in the brain. In a more translational approach we will also test pharmacological interventions that may open new possibilities for therapeutic approaches in patients.