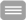Pneumonia reflects a frequent clinical condition that may lead to lung barrier failure, bacteremia, and sepsis, including local (ARDS) and remote organ dysfunction. Underlying infections are often caused by Streptococcus pneumoniae, a Gram-positive pathogen that produces pneumolysin as a virulence factor. Pneumolysin, a cholesterol-binding pore-forming toxin, may trigger barrier failure and the onset of sepsis. We have shown that changes in sterol biosynthesis in cells of the liver (hepatocytes), in particular cholesterol biosynthesis, are induced as a remote adaptive response to circulating pneumolysin. Indeed, a communication between the infection of the lung and the liver occure. It was shown that an increased level of cholesterol in human is associated with a reduced severity of infections. The therapeutic potential of interfering pathways is unexplored. However, even simple delivery of cholesterol, a detergent, to the lungs poses significant hurdles. We propose to design and monitor interventions to prevent local and remote organ failure using cutting-edge technologies, such as recently developed organ-specific nanoparticles, tranporting drug to hepatocytes, and systems biology approaches for transcriptome and metabolome analysis, respectively, to answer whether selectively targeting the cholesterol pathway can improve lung function during pneumococcal disease and prevent septic disease progression and remote organ failure.